If your teenager’s feet are staging the same itchy rebellion every few weeks, you’re not imagining it—athlete’s foot is the sort of uninvited guest that loves a warm trainer and a busy changing room. It’s common, contagious, and—crucially—often under-treated, which is why it keeps finding its way back like a bad song on a playlist.
To cut through the confusion (and the scratching), we spoke to Emma McConnachie, podiatrist and vice-president of the College of Podiatry, for a straight-talking guide to spotting, stopping, and preventing recurring flare-ups.
What athlete’s foot actually is (and why it spreads so easily)

“Athlete’s foot (or as it is also known, ‘tinea pedis’) is a very contagious fungal infection that is picked up by coming into contact with infected tissue (like skin),” says McConnachie.
That’s the heart of it: fungus doesn’t need a grand invitation. It just needs access—shared floors, damp socks, skin contact—and enough time to settle in.
And the tricky bit? It doesn’t always look the way people expect.
“Athlete’s foot isn’t easy to spot, as the symptoms are not always consistent and can look quite different.
Your feet could be itchy, with little bubbles of fluid, or with red pin-pricks in the skin. Or alternatively, it could look like very dry and flaky skin – on just one or both feet. All of these symptoms are usually seen in the arch of the foot or around the toes.
“Large, painful cracks can also develop, and the condition can spread to all toes or even the soles of the feet if left untreated. After several months, athlete’s foot can spread into the toenails and cause permanent damage, so it’s always best to seek treatment as quickly as possible.”
Translation: it can masquerade as “just dry skin,” then quietly graduate into something that’s harder to shift—especially if it reaches the nails.
Who gets athlete’s foot most often (and why teens are prime targets)
“Not everyone who comes into contact with the infection will get it, but those with moist, sweaty feet, or very dry feet with breaks in the skin, are most likely to develop it. In fact, it’s called athlete’s foot as people wearing sweaty trainers all day are also at a higher risk of getting infected!
“Another very common way to develop athlete’s foot is by walking barefoot in places that other people do, such as communal showers and changing rooms. Athlete’s foot can also be passed on through contact with others, however, people who sweat more are at increased risk.”
Teenagers, for all their gifts, are not widely celebrated for meticulous shoe rotation or the gentle towel-drying of every toe. Add sport, school changing rooms, synthetic footwear, long days, and the habit of kicking trainers into a dark corner to “air out” (meaning: never), and you’ve got perfect conditions.
The risk factors are boring but decisive: moisture, friction, tiny skin breaks, and repeated exposure.
How to stop athlete’s foot coming back
Prevention is not glamorous. It’s also the part that most people skip—then wonder why athlete’s foot returns on schedule.
“To help prevent fungal infections, you can follow these top tips: Regularly change up which shoes you wear, to give them time to dry out properly, or at least ventilate or dry your shoes.
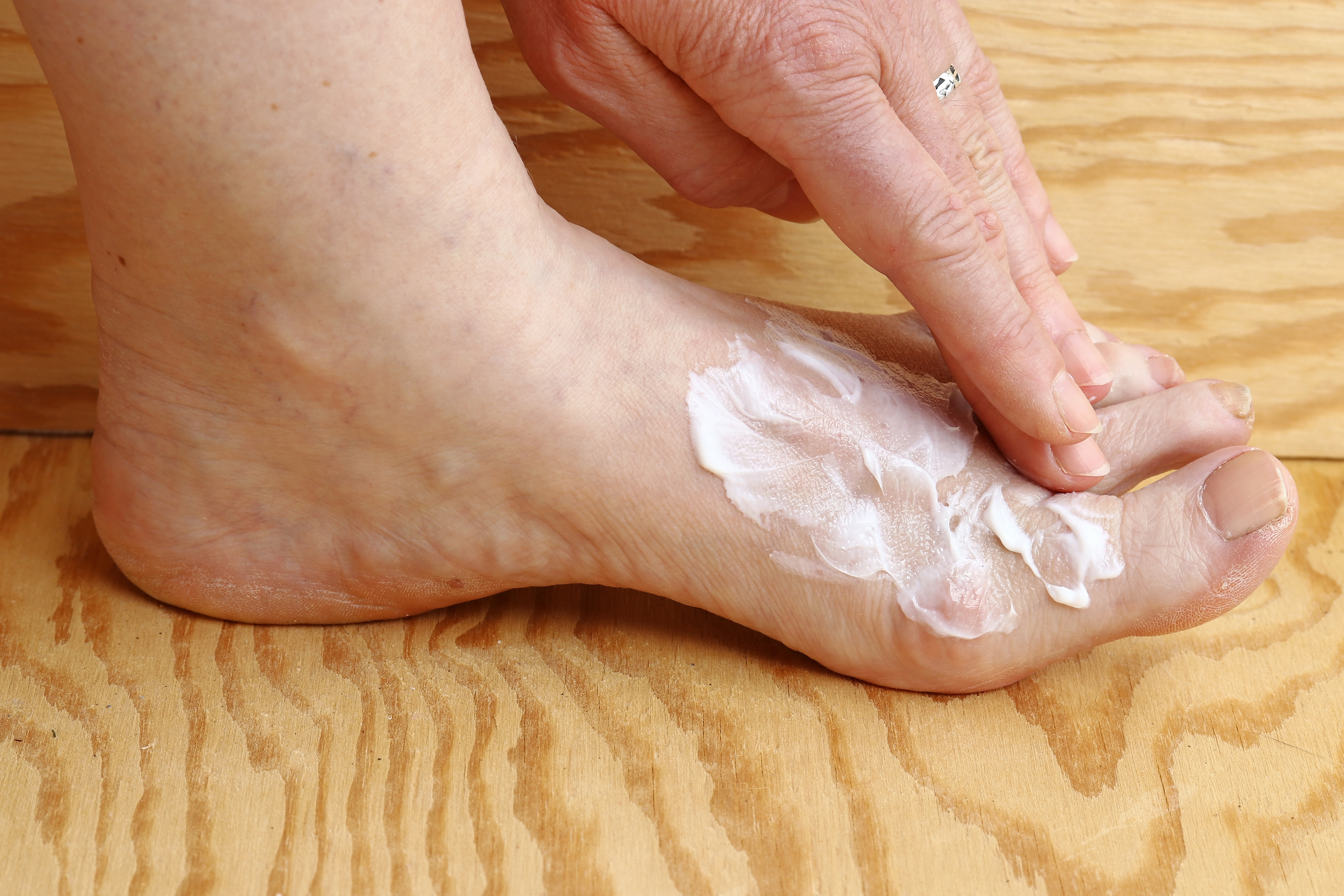
“Always dry between your toes after bathing and avoid applying creams in between your toes. It’s easy for it to get too moist in there and for the skin to crack, which increases your risk of infection. However, do moisturise your feet regularly, especially the heels, as they can easily split from being too dry.
“Avoid walking barefoot in communal areas. Flip-flops and pool shoes are easily available and the old-fashioned white ‘verruca sock’ has also had a modern makeover! Neoprene style swim shoes are also now available in a variety of colours and styles, with the added bonus of a thin, non-slip sole – ideal for at the pool!
“Make sure your toes aren’t squeezed together in tight shoes, and instead look for shoes which have room for your toes to move – preferably made from natural materials. And don’t try on shoes barefoot in shops. I recommend always taking a pair of socks or thin knee-high hosiery with you when you try on potential shoe purchases.”
A few points worth underlining for real life:
- Shoe rotation is not optional. Damp shoes are a fungal spa.
- Dry between the toes. That little fold of skin is where trouble likes to live.
- Moisturise—strategically. Heels cracking is an open door; too much moisture between toes is another.
- Barrier footwear in communal areas. Yes, even if they “only popped in for a second.”
- Toe room matters. Cramped toes increase rubbing and keep things sweaty.
This is the unsexy truth: recurrence usually isn’t bad luck—it’s environment + habit.
Treating athlete’s foot: what works from the pharmacy
Over-the-counter options can be highly effective, especially when started early and used properly.
“There are many effective over-the-counter treatments for athlete’s foot, including creams and sprays, which can range from requiring just a single application to applying them every day for a couple of weeks. Make sure to use these on both feet, as the fungus can be in areas that don’t look affected.
“For nail infections, consult with a podiatrist, who will be able to determine if it is a fungal infection or just a discoloured nail, and can recommend treatments appropriate for your medical history.”
Two common mistakes keep athlete’s foot on a repeat loop:
- Stopping too soon because it “looks better.”
- Spot-treating only the obvious patches, leaving microscopic fungus behind.
If nails get involved, the stakes rise: nail infections can be stubborn, and guessing rarely helps.
When recurring athlete’s foot needs professional help
There’s a point where persistence stops being “normal” and starts being a sign that something’s been missed—wrong diagnosis, resistant infection, reinfection from footwear, or spread beyond the original area.
“As it is a fungal infection, it’s important to treat athlete’s foot early to prevent longer-term damage, or spreading to other areas of your skin. If simple treatments don’t work within three weeks, or you spot anything you are unsure about, then you should visit a specialised healthcare professional, such as a podiatrist. You can find a local podiatrist via the College of Podiatry website (cop.org.uk).”
Three weeks is a useful, practical line in the sand. If it’s not improving, don’t keep waging a private war with half-measures.
The bottom line
Athlete’s foot thrives on two things: quiet neglect and damp routine. The good news is that prevention is rarely complicated—just consistent. Dry thoroughly, rotate shoes, protect feet in communal spaces, and treat early and properly.
And if your teenager rolls their eyes at the mention of flip-flops in the changing room, remind them: dignity is temporary. Fungal infections have patience.







